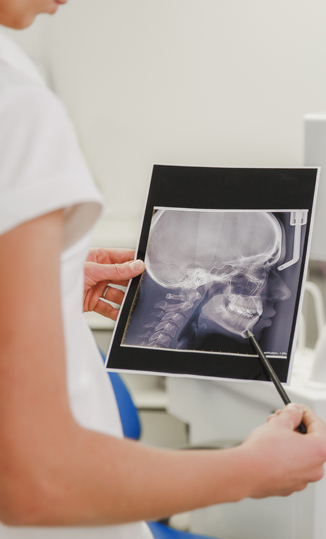
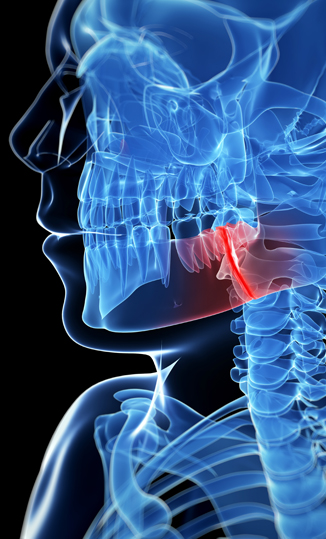
Patients frequently present with concerns about jaw joint pain, stiffness with movement of the lower jaw and jaw joint noises. The biological name for the jaw joint is the temporomandibular joint and thus problems related to jaw joint function are referred to as temporomandibular joint disorders (TMD). Dentists will sometimes refer to jaw joint issues as TMJ problems but the correct term is TMD.
The term TMD refers to a group of disorders that affect the jaw joints and the associated jaw muscles. Although patients often assume that all these problems are the same for each patient, the reality is that many different types of jaw joint disorder can occur. Simple overuse of the joint from constant chewing during the day or grinding of teeth at night time, may cause soreness and joint inflammation. This problem is generally easily managed with treatments such as:
-
jaw rest and a soft diet;
-
oral anti-inflammatory medication;
-
hot or cold packs on the painful joint;
-
use of anti-inflammatory creams on the painful area; and,
-
use of a night-time bite splint.
On rare occasions, jaw joint pain may be persistent and more invasive treatments like pain killing injections or jaw joint surgery may be required.
The strategy for treating jaw pain that is mostly muscular is slightly different. For example, rather than resting the jaw, the patient is encouraged to carry out stretching exercises. If the hinge joint (i.e., the temporomandibular joint) is not inflamed, then simple stretching of the lower jaw into the wide open position (as in yawning for example) can provide significant relief from jaw soreness. One of the interesting things about jaw muscle pain is that it can mimic toothache. This sometimes happens when inflamed muscle tissue refers pain into the adjacent teeth. The pain can appear to be just like a toothache, e.g., when you have a cavity or damage to your tooth. A good clinical examination will help to distinguish between jaw muscle pain and ordinary toothache.
Jaw joint clicking is a common complaint. This phenomenon is more frequently seen in female patients and in most cases does not require treatment. However, there are circumstances in which the clicking joint needs to be treated. In circumstances where the jaw joint clicking is becoming painful or stiff, we can consider specific treatment approaches to alleviate the symptoms. Some of the treatment items mentioned above such as bite splints, oral anti-inflammatories, and exercise programmes, etc., may be helpful.
A small percentage of patients with clicking joints will progressively deteriorate to the point where the jaw joint itself becomes stiff or locked. This more difficult scenario is often characterised by painful chewing. These symptoms may occasionally resolve spontaneously, but in most cases direct intervention is required. Treatment may include jaw joint injections or surgery, or the use of a bite splint at night time.
Jaw joint locking can occur for a variety of reasons, the most common of which is movement or displacement of the disc within the jaw joint. The disc is a small piece of cartilage which is usually located between the bones in the joint and acts as a separator or stabiliser in jaw movements. This disc tissue may slide or move out of place in adulthood without causing a problem for the patient, but in some patients this phenomenon occurs in a way that causes pain and stiffness, which can be quite severe.
Sometimes we see more unusual problems like arthritis and other degenerative diseases but these issues are relatively rare in comparison to the more common problems like jaw soreness and stiffness.
However, the main thing to remember about jaw joint problems is that the success rate in treating them is very high. Jaw joints have a great capacity to repair, unlike some other tissues.
If you have problems relating to Sleep apnoea and would like more information, click here to read about sleep apnoea and snoring devices that may help.